Bradley Corallo, Jennifer Tolbert, Patrick Drake, Sophia Moreno, and Robin Rudowitz
Jan 30, 2024 - KFF
Ten months into the unwinding of the Medicaid continuous enrollment provision, states are continuing to reverify the eligibility of the roughly 94 million enrollees in the program. KFF tracking shows that states have reported outcomes for roughly half of the people expected to undergo renewals during the unwinding period. This policy watch examines the latest data and key issues to watch during the next phase of the unwinding.
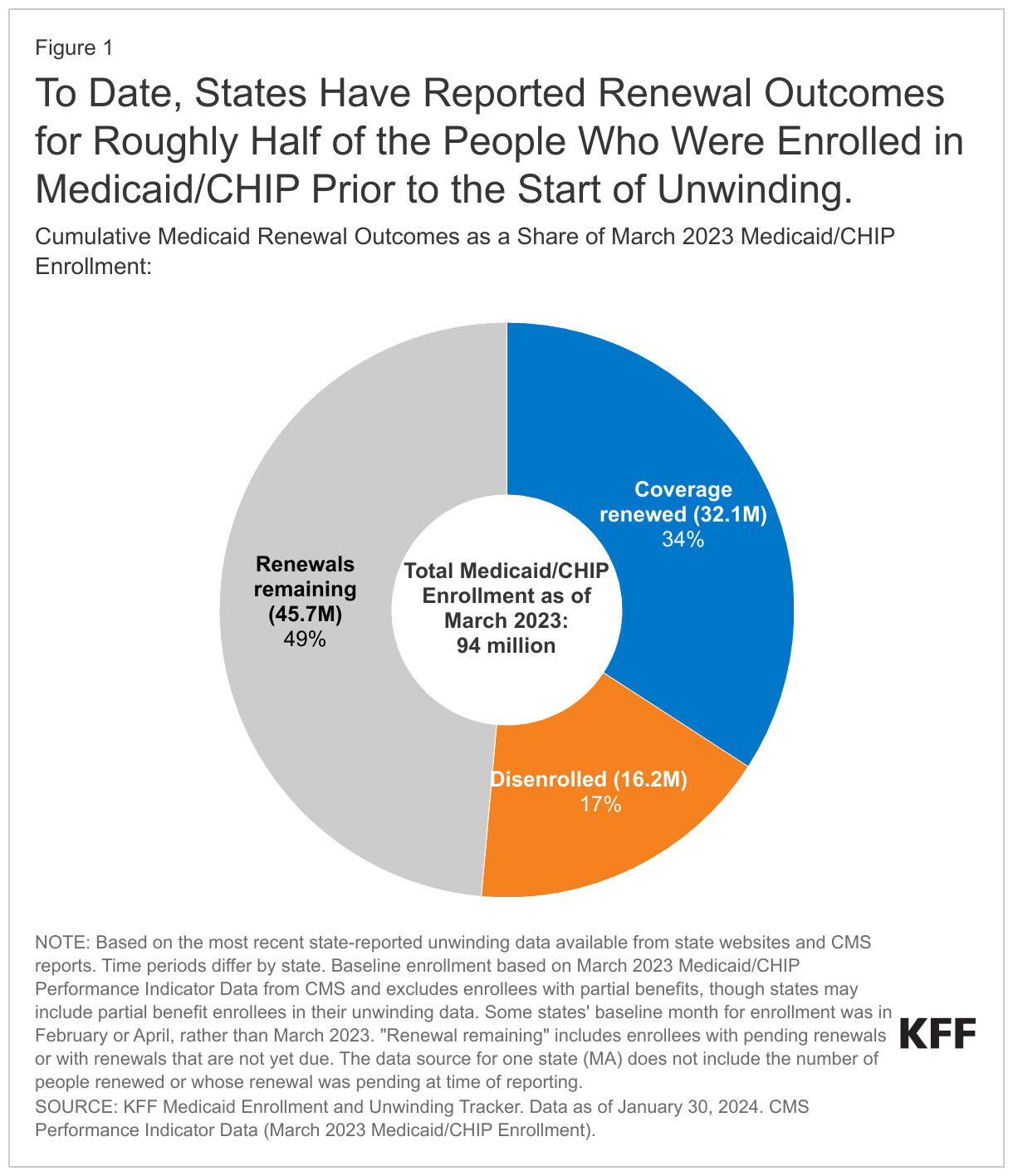
As of the end of January 2024, states have reported renewal outcomes for half of all enrollees, including 34% (32.1 million) who have had their coverage renewed and 17% (16.2 million) who have been disenrolled (Figure 1). Due to lags in data reporting, which vary from one to three months across states, the number of completed renewals is an undercount. Prior to the start of the unwinding, KFF projected that 17 million people would be disenrolled during the unwinding based on state estimates, but noted the range could be 8 to 24 million people disenrolled because of the uncertainty and expected variation across states. Given how many renewals are left to complete, disenrollments are highly likely to exceed 17 million.
There is significant variation in the share of completed renewals across states, ranging from 87% in Oregon to 22% in Wyoming (Figure 2). Some of this variation reflects when states resumed disenrolling people as well as differences in the pace of processing renewals. But actions some states have taken in response to inappropriate or high procedural disenrollment rates are also a factor. In August and September, 30 states were required to reinstate coverage and temporarily pause disenrollments for some enrollees to address non-compliance with federal rules. Some states also voluntarily extended renewal deadlines to delay procedural disenrollments while they conduct additional outreach to enrollees. Finally, the variation across states also reflects differences in how states report unwinding data and the frequency of updates.
Since the start of unwinding, Medicaid enrollment has declined in every state, ranging from 32% in Idaho to 1% in Maine (Figure 3). Overall, the Medicaid enrollment has declined by nearly 10% across states since the start of unwinding. The enrollment declines shown here are measured against each state’s baseline enrollment, which is enrollment in the month prior to when the state resumed disenrollments and which varies by state. Due to the lags in reporting, current enrollment declines are greater in some states. Changes in enrollment reflect the people who disenroll from Medicaid as well as those who newly enroll, and those who re-enroll within a short timeframe following disenrollment, also known as “churn.” Two states, South Dakota and North Carolina, implemented the Medicaid expansion since the start of unwinding (in July and December 2023, respectively), which should mitigate enrollment declines in these states.
Disenrollment rates could moderate in the second half of the unwinding as states continue efforts to reduce procedural disenrollments and because some states have worked through “likely ineligible” populations. Many states continue to adopt flexibilities during the unwinding to improve ex parte renewal processes, which reduce paperwork burden on enrollees and can reduce procedural termination rates. In addition, some states have worked through renewals for people the state flagged as likely ineligible, who the states prioritized for renewals early in the unwinding. The remaining population in these states is more likely to still be eligible and, therefore, less likely to be disenrolled. For example, Arkansas and Idaho recently announced that they completed renewals for “likely ineligible” enrollees after six months of unwinding, and the number and rate of disenrollments declined in subsequent months (the total number of renewals also declined steeply in both states).
The unwinding’s implications for broader coverage trends are not yet known. There is currently limited data on how many people losing Medicaid are reenrolling in Medicaid, transitioning to other sources of health coverage, including employer coverage and coverage through the Affordable Care Act (ACA) Marketplaces, or becoming uninsured. Data for 2022 showed the national uninsured rate had dropped to 7.9%, the lowest level on record. While the unwinding will likely contribute to increases in the number of people who are uninsured and in the uninsured rate, it is unclear what the magnitude of these increases will be. Federal survey data will not be available to understand these trends until well after the unwinding period ends, and surveys that rely on self-reported health insurance status significantly undercount Medicaid enrollment. In the meantime, state and national administrative data on ACA Marketplace enrollment and private insurance coverage can shed some light on the coverage picture. However, while national data show record enrollment in Marketplace coverage, Medicaid unwinding is only one factor contributing to that growth and a relatively small share of people disenrolled from Medicaid are transitioning to Marketplace or Basic Health Plan coverage. It will be some time before there is a more complete picture at the national level of how many people losing Medicaid find other coverage or become uninsured.